Ozempic, Wegovy, and other GLP-1 weight loss drugs have become the talk among people who want to lose weight. They started out as drugs to manage type 2 diabetes. While they’re still…
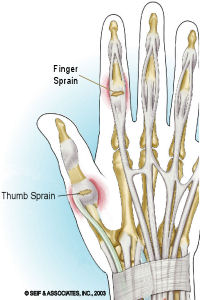
A sprained finger is common in sports with the most common injury being a sprain to one of the ligaments located within the finger. Each finger has three small bones (phalanges) separated by two interphalangeal joints. The thumb is unique and has one interphalangeal joint and only two small phalange bones.
A sprain is an injury to a ligament. Each of the joints located in the finger has collateral ligaments that run along each side of the joints. It is these collateral ligaments that are commonly sprained in sports. Athletes in sports that use balls are the most at risk for a sprained finger including athletes competing in the sports of basketball, baseball, and softball.
A sprained finger is classified from mild to severe and is diagnosed as first-degree, second-degree, or third-degree sprains.
Is considered mild because the ligaments are only stretched and not torn. The athlete may complain of localized swelling and pain around the injured joint. The athlete’s ability to flex and extend the finger may be somewhat limited due to the swelling within the joint. Last, the strength of the finger is usually not affected.
In most first degree sprains, the athlete is able to continue participating in sports. However, the athlete may benefit from taping the injured finger to an adjacent finger to prevent further injury.
Results in more damage to the ligament and may also include damage to the joint capsule as well. Because the force of the injury is stronger, the resulting damage may include a partial tear of the ligament and associated joint capsule.
This type of injury results in significantly more swelling and pain. The swelling may extend throughout the finger within the first few hours possibly limiting the range of motion of both joints within the finger. The joint may also be tender to touch specifically over the injury site.
The primary difference between a first and second-degree sprain is that there will be laxity in a second-degree sprain when the ligament is tested. This means that when a ligament test is performed on an athlete with a first-degree sprain, the ligament will be tight. However, a ligament stress test performed on an athlete with a second-degree sprain will result in a visual opening of the joint line, but there will be an end point indicating that the ligament is only partially torn.
Is the most severe sprain resulting in a complete rupture of the ligament. A full ligament rupture usually occurs at its attachment, but may also occur in the middle of the ligament. In some cases, the bone can actually be pulled away from the distal attachment causing an avulsion fracture.
A third-degree sprained finger is often associated with a subluxation or dislocation of the finger. A subluxation is a partial dislocation that reduces itself and the athlete may not even realize that it has occurred.
An athlete will notice a dislocation of the finger because of the amount of pain and obvious deformity of the finger. The initial instinct of the athlete is to pull on the finger to reduce the dislocation. Even if the athlete reduces the dislocation, the athlete should still be splinted and referred for an x-ray.
A third-degree sprain will result in laxity and instability of the finger with severe swelling, pain, and possibly discoloration. All athletes with a suspected third-degree sprain need to have the finger splinted and then be referred for an x-ray to rule out a possible fracture.
A sports medicine professional can diagnose a sprained finger given a thorough medical history and comprehensive physical assessment. If a third-degree sprain is suspected, an x-ray can be ordered to rule out a possible fracture.
The most common mechanism of a sprained finger is a blow to the end of a finger caused by a ball traveling at high speed. An example is a basketball player mishandling a pass and catching it off the end of the finger or a baseball player taking a bad bounce off of a groundball and having the ball strike the end of the finger.
The force of the blow at the end of the finger reverberates up the finger to the joint causing the joint to either hyperextend or move sideways. Either one of these movements can injure the collateral ligaments in the fingers.
Another mechanism of injury in sports is catching a finger in a jersey or piece of sports equipment. If the force is stronger than the tensile strength of the ligament, the ligament can be stretched or torn.
Once a fracture has been ruled out, sports injury treatment using the P.R.I.C.E. principle should be utilized. Ice can be applied for twenty minutes every two hours either through the use of a small ice pack or cold water immersion.
Coldwater immersion is an effective treatment for a sprained finger because the cold water can surround all of the injured area rather than just one side of the finger as in the application of an ice pack. Coldwater immersion can easily be accomplished with the use of a large cup, water, and the addition of some ice.
An athlete with a second-degree sprain should have the finger splinted by either buddy taping the injured finger to the adjacent finger or by utilizing an aluminum splint. The finger should be splinted so that the injured joint and adjacent bones are immobilized. Aluminum splints can be custom cut to fit and bent to accommodate most finger injuries.

Because there is more tissue damaged in a second-degree sprain, the finger will swell more and may have some discoloration. As in a first-degree sprain, the athlete should utilize the P.R.I.C.E Principle for the first 48-72 hours.
As the swelling begins to diminish, the athlete can begin gentle range of motion exercises to begin to regain the flexibility of the finger. This can be accomplished using a number of different items including a tennis ball, racquetball, or rolled sock.
The athlete places the object in his/her hand and gently squeezes. This exercise increases both the range of motion of the joint plus the strength of the muscles in and around the injured joint. The athlete gradually squeezes the ball and then relaxes. This can be performed ten times every hour.
Care should be taken for the athlete not to squeeze so hard that it causes pain. As the ligament and tissue heal, the athlete can gradually increase the intensity of the grip on the ball.
An athlete with a third-degree sprain should be seen by a sports medicine physician and may need to have the injury surgically repaired.
Hundreds of athletes sustain acute injuries every day, which can be treated safely at home using the P.R.I.C.E. principle. But if there are signs or symptoms of a serious injury, emergency first aid should be provided while keeping the athlete calm and still until emergency service personnel arrive. Signs of an emergency situation when you should seek care and doctor treatment can include:
In addition, an athlete should seek medical care if acute symptoms do not go away after rest and home treatment using the P.R.I.C.E principle.
Because long term swelling is fairly common in sprained fingers, gaining full flexibility can take a long time. In some cases, the joint can look swollen for up to one year post-injury.
Most athletes return fairly quickly to sport after a sprained finger, but will utilize a buddy tape job to protect the finger from further injury. The finger should be taped to an adjacent finger above and below the injured joint with ½ inch athletic tape. This ensures that the joint is protected, but also allows the athlete to flex and extend his/her fingers as needed.
Question: How do you know if your finger is sprained?
Answer: A sprained finger will have pain and swelling around the injured joint with stiffness when trying to move.
Question: How long does a sprained finger take to heal?
Answer: The healing time for a finger sprain is dependent on the severity of the injury. A Grade 1 sprain will start to feel better in 3-5 days and can successfully recover in 2-4 weeks. A grade 3 finger sprain is the most severe sprain resulting in a complete rupture of the ligament and can take several months to heal.
Question: What does a sprain feel like finger?
Answer: A sprained finger will have pain and swelling around the injured joint with stiffness when trying to move.
Question: Can a sprained finger heal on its own?
Answer: Yes, sprained fingers can heal on their own but it does depend on the severity of the injury. Mild finger sprains usually improve in a few days with basic care and heal entirely after a few weeks of Protection, Rest, Ice, Compression, and Elevation (P.R.I.C.E) .
Mallet finger is not a sprain, it’s a complete disruption of the tendon that straightens the joint at the tip of the finger. Tendon can be avulsed (pulled off) from the bone or simply tear. Surgery is an option for quicker stabilization (we regular people wear a splint for 8 wks) https://t.co/GE4ntdtCaJ
— DocFlynn (@DocFlynnNFL) October 8, 2021
NBA started tracking shots in 1996-97.
Michael Jordan played through a badly sprained wrist and dislocated index finger in 1997-98. He suffered permanent damage to that finger in January 1999.
From 1996-2003, MJ ranked #1 in clutch shooting with 5 seconds left…9-22, or 40.9%. pic.twitter.com/CSeePIO529
— AirJordans23 (@AirJordans2323) January 11, 2023

Ozempic, Wegovy, and other GLP-1 weight loss drugs have become the talk among people who want to lose weight. They started out as drugs to manage type 2 diabetes. While they’re still…

Athletes tend to do a good job of training their muscles, heart and lungs. But some of them (particularly endurance athletes and those in running sports) commonly fail to train their gut.…

GLP-1 drugs aren’t new on the market. They’ve been around to help people manage type 2 diabetes by mimicking the activity of the GLP-1 hormone. Recently, the drug has become a popular…

Key Takeaways Resistance training and high protein intake are non-negotiable requirements to preserve muscle during treatment. GLP-1’s can blunt the thirst mechanism and athletes are at high risk for dehydration and electrolyte…

Nutrition for injury recovery is often overlooked but a key element to faster recovery. Lets face it, athletes get injured and it’s part of the deal. Be it a torn ACL, Achilles…