Neck Strain
Last Updated on August 12, 2024 by The SportsMD Editors
A neck strain is a painful and debilitating injury because the pain and associated muscle spasm can inhibit any and all movements of the head/neck. For an athlete who needs to have full movement of his/her head, a neck strain can sideline an athlete until the injury has healed. Athletes who try to play through the pain of a neck strain may inadvertently prolong the healing process.
A strain is an injury to a muscle. A strain to a neck muscle can include any of a number of either deep or superficial muscles located around the neck. The muscles of the neck are responsible for the following movements including flexion (chin to chest), extension (eyes to ceiling), rotation, and lateral flexion (ear to shoulder).
When any one of these muscles becomes injured, the movements of the head can become severely limited because strained muscles often result in associated muscle spasms in the injured or surrounding muscles.
While a strain is a tear to the muscle fiber, a spasm is an involuntary contraction of the muscle that tightens the muscle to a point where movement is not possible. Muscle spasm is a mechanism of the body to protect injured or weakened muscles and often accompanies a muscle strain.
Classifications of neck strains
Muscle strains are classified as mild (first degree), moderate (second degree), or severe (third degree) depending on their severity.
First degree neck strain:
Are the result of a stretching of the muscle tissue that results in pain, tightness, and discomfort with movement of the head/neck. Depending on the muscle that is affected, some or all movements of the head/neck may be painful for the athlete.
Moderate or second degree neck strain:
Muscle strains are caused by the actual tearing of some of the muscle fibers within the muscle. This can result in increased pain, muscle spasm, swelling discoloration, and increased limitations on head/neck movement.
Third degree or complete tear:
The most severe type of muscle strain is the result of a complete tear of the muscle usually at the place in the muscle where the muscle and tendon connect or at the insertion of the muscle into the bone.
This type of injury is a serious injury that may result in deformity of the muscle, intense pain, disability, muscle spasm, swelling, and discoloration. Any athlete suspected of a third degree muscle strain should be immobilized and immediately referred for medical evaluation and treatment.
Diagnosing neck strain
A neck strain can be easily diagnosed by a medical professional with a thorough medical history and the administration of a clinical evaluation. If other injuries may be suspected, the physician may order an x-ray or MRI to rule out a bone, spinal cord, or disc injuries.
Who gets neck strains?
One of the most common mechanisms of injury for a neck strain is a “whiplash-type” of injury similar to that seen in individuals who have been rear-ended in car accidents. However, in sports, the whiplash occurs when the head is snapped forward and then backward either as a result of contact with an opponent or with the ground.
This type of injury can be seen in athletes in a number of sports including soccer, basketball, wrestling, and football. Because the head is used as a sports implement in soccer, these athletes are more at risk for a neck strain.
Causes of neck strain
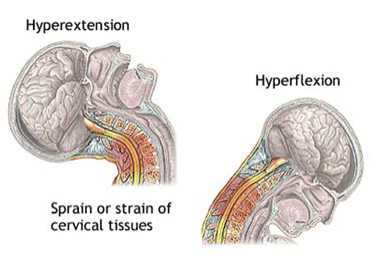
Besides a “whiplash” mechanism, a neck muscle can be strained anytime the force of resistance is stronger than the muscle itself. For example, a baseball or softball player can sustain a neck strain when sliding headfirst into a bag if his/her head is stopped by the opponent while the momentum of the athlete’s body continues to move forward thus straining the side muscles of the athlete’s neck.
A neck strain can also occur in a head-to-head contact in football if the players’ sizes are unequal. The smaller athlete’s head may be forced to one side resulting in a strained muscle on the opposite side of the neck.
Last, a fall from any height greater than that of the athlete can result in a neck strain secondary to other more severe neck injuries including fracture, cervical spinal cord injury, or disc injury. In any serious neck injury, critical injuries must be ruled out first.
Preventing neck strain
Athletes engaged in contact sports should regularly work on neck strengthening muscles. Muscles that are stronger are better able to withstand greater forces without being injured.
Resistance exercises should be performed to strengthen all of the motions of the neck including flexion, extension, rotation, and lateral flexion. This can be accomplished with manual resistance provided by the athlete (or a buddy) or by a custom designed piece of equipment.
Athletes on contact sports or in sports in which a lot of stress is placed on the head/neck (wrestling) should maintain a strength training program year round to ensure that the muscles are as strong as possible when the athlete needs to compete. This type of proactive strength training program can go a long way to preventing neck muscle strains in contact sports.
Attention to proper mechanics is another key to preventing neck muscle injuries. Ensuring that athletes are taught to not lead with their heads in contact sports is one way to reducing head and neck injuries.
Treatment for neck strain
Acute neck muscle strains should be treated with the P.R.I.C.E. principles – Protection, Rest, Icing, Compression, Elevation – to reduce pain and swelling and reduce secondary injury. Ice packs can be applied to the injured muscle for twenty minutes every two hours for the first two to three days.
Resting the neck muscles is the most important component of treatment in the early healing process. This can be accomplished through the use of a soft collar. The soft collar is designed so that the chin can rest on the front of the collar allowing the muscles surrounding the neck to relax.
The athlete needs to understand that the healing process will take longer if the neck muscles are continuously engaged and contracted (as in holding the head up). The neck muscles will still heal in time, but resting the muscles allows for much quicker healing.
The only other way to rest the muscles of the neck is bed rest. When the head is resting on a pillow, the neck muscles can be at rest. Anytime the athlete is sitting, standing, walking or active, the neck muscles are contracted to keep the head upright.
So if the athlete needs to be active during the day (i.e., attend classes, work, etc.), the athlete should wear a soft collar. The collar should be worn as long as the athlete has pain with any movement of the head (usually a couple of days).
After a couple of days of cryotherapy, the athlete can apply hot packs (moist or dry heat) to the injured area for 10 – 15 minutes at a time. This can be repeated throughout the day as needed.
The heat is effective at reducing muscle spasms and increasing circulation to enhance the body’s own healing process. The relaxation effect of heat can also help relax tight muscles so that the athlete can begin to move his/her head through increasing ranges of motion.
For moderate to severe injuries, a physician may recommend a prescription muscle relaxant or an over-the-counter NSAID to help reduce pain and discomfort.
Once the pain and stiffness begin to decrease, the athlete can begin to work on neck stretching exercises to gain his/her range of motion back. These exercises can be done by the athlete at home. Each can be performed for 20 to 30 seconds and repeated three times.
Increasing neck flexion can be accomplished by having the athlete move his/her chin to the chest until tightness is felt and then placing his/her hands on the back of his/her head. The athlete can then apply pressure pushing the head further into flexion.
Lateral flexion left and right can be increased by having the athlete tilt his/her head sideways trying to touch his/her ear to the shoulder. To enhance the stretch, the athlete can place one hand on the top of the head and place light pressure on the head pulling the ear closer to the shoulder. This stretch should be repeated for both the right and left sides.
Rotation left and right can be increased by turning the head towards the shoulder (opposite the side that is tight) and increasing the stretch by applying additional pressure (by the hand) in the direction of the shoulder at the chin. This stretch can be done for both sides of neck rotation.
After stretching exercises have been completed, the athlete can add strengthening exercises by applying resistance with his/her hands to the head. Because these exercises are done manually, the athlete can perform 3 sets of 10 repetitions for each exercise.
To increase strength of the muscles that extend the head/neck, the athlete needs to start with his/her chin on the chest, place his/her hands on the back of the head, add resistance by pulling, and then slowly extend the head until the eyes are facing the ceiling.
To increase the strength of the muscles that flex the head/neck, the athlete needs to start with the head fully extended (eyes to the ceiling), place his/her hands on the forehead, apply resistance by pushing against the forehead, and then slowly flex the head moving the head forward until the chin is on the chest.
Muscles for head/neck rotation can be strengthened by beginning with the head fully rotated (either right or left with chin over the shoulder) and applying pressure against the chin while the athlete rotates his/her head through the full range until the chin is directly over the opposite shoulder.
Treating neck strain with KT Tape:
Last, the muscles that laterally flex the head/neck can be increased by relaxing the head/neck and placing the ear towards the shoulder until tight (either right or left), applying resistance with one hand at the side of the head, and slowly moving the head up and over towards the opposite shoulder. This exercise can be repeated for both sides.
Recovery – Getting back to Sport
The athlete can begin functional sports specific exercises when he/she has a full range of motion and full strength in all directions of the head/neck without pain. Functional exercises should mimic the skills that the athlete will need to perform when he/she returns to sport.
Whatever the athlete’s sport, each component of the sport should be included in some type of functional exercise to ensure that the athlete can complete every skill without pain prior to returning to sport.
Good functional drills can begin with regular warm-up drills for the sport. They should include both lower and upper extremity work and should begin at a low intensity (50%) and gradually increase (to the athlete’s tolerance) to full intensity over time.
Once the athlete can complete full intensity functional drills without any pain, the athlete is ready to return to sport. If pain returns when the athlete is performing sport specific drills, then the athlete should stop the activity and apply ice. When the athlete is once again pain-free, he/she may begin functional exercises again.
When Can I Return to Play?
The athlete can return to sport when he/she has been released by his/her physician and has full range of motion, full strength, and has completed full intensity functional training without pain.
Getting a Second Opinion
A second opinion should be considered when deciding on a high-risk procedure like surgery or you want another opinion on your treatment options. It will also provide you with peace of mind. Multiple studies make a case for getting additional medical opinions.
In 2017, a Mayo Clinic study showed that 21% of patients who sought a second opinion left with a completely new diagnosis, and 66% were deemed partly correct, but refined or redefined by the second doctor.
You can ask your primary care doctor for another doctor to consider for a second opinion or ask your family and friends for suggestions. Another option is to use a Telemedicine Second Opinion service from a local health center or a Virtual Care Service.
Get a Virtual Sports Specialized appointment within 5 minutes for $29
 When you have questions like: I have an injury and how should I manage it? How severe is it and should I get medical care from an urgent care center or hospital? Who can I talk to right now? SportsMD Virtual Urgent Care is available by phone or video anytime, anywhere 24/7/365, and appointments within 5 minutes. Learn more via SportsMD’s Virtual Urgent Care Service.
When you have questions like: I have an injury and how should I manage it? How severe is it and should I get medical care from an urgent care center or hospital? Who can I talk to right now? SportsMD Virtual Urgent Care is available by phone or video anytime, anywhere 24/7/365, and appointments within 5 minutes. Learn more via SportsMD’s Virtual Urgent Care Service.
References
- Bahr, R. & Maehlum S. (2004). Clinical Guide to Sports Injuries. Human Kinetics: Champaign, IL.
- Brukner, P. & Khan, K. (2002). Clinical Sports Medicine (2nd Ed.). McGraw Hill: Australia.
- Rouzier, P. (1999). The Sports Medicine Patient Advisor. SportsMed Press: Amherst, MA.

