Dislocated elbow
Last Updated on August 12, 2024 by The SportsMD Editors
Several types of dislocations can occur in the elbow. In young children, the most common dislocation is a dislocation of the proximal head of the radius. This type of dislocation is also referred to as “nursemaid’s elbow” and “pulled-elbow syndrome” because it is commonly caused when an adult swings a child by their arms. In teenagers and young adults, the most common dislocated elbow is a posterior dislocation of the ulna. This can be a very serious injury depending on the number of structures involved. A complex dislocation can possibly be career-ending for an athlete.
The elbow is actually comprised of three joints with differing combinations of the 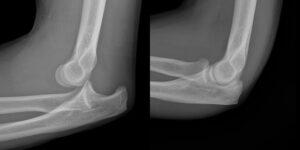 humerus, ulna, and radius. The primary elbow joint is the humeroulnar joint. This joint is responsible for flexion and extension of the elbow. A dislocation of the ulna posteriorly from the humerus can be considered a catastrophic injury because of the abundance of nerves and blood vessels that can be damaged within the anterior elbow.
humerus, ulna, and radius. The primary elbow joint is the humeroulnar joint. This joint is responsible for flexion and extension of the elbow. A dislocation of the ulna posteriorly from the humerus can be considered a catastrophic injury because of the abundance of nerves and blood vessels that can be damaged within the anterior elbow.
Allowing the forearm to pivot and turn the hand up and down is the radioulnar joint. If the radius is injured (as in a radial head dislocation), the athlete would have significant pain trying to rotate his/her hand.
Classifications of a dislocated elbow
A dislocated elbow in actuality is a third degree ligament sprain (rupture of one or more ligaments) of the stabilizing ligaments that surround the humeroulnar joint. There are simple dislocations (no fractures involved), and more complex dislocations (associated fractures).
Along with possible partial and/or full ruptures of the medial and lateral collateral ligaments (ligaments that run alongside the elbow), dislocations can be associated with fractures including fractures of the radial head (5% – 10%), avulsion fractures of the medial and lateral humeral condyles (12%), and fractures of the coronoid process (10%) (Bahr & Maehlum, 2004).
The major complication with a dislocated elbow is if the nerves and blood vessels are compromised because of the bone disruptions. If the pulse is absent in the wrist and hand, the dislocation needs to be reduced immediately to save the integrity and tissues of the muscles and other soft tissue structures.
Signs and symptoms:
• Snapping or cracking sensation
• Immediate, severe pain
• Rapid swelling
• Total loss of function (inability to move or use the elbow and hand)
• Obvious deformity
• The elbow is slightly flexed and supported by the uninjured arm.
• Numbness and/or weakness of the hand and fingers
Who gets a dislocated elbow?
It takes a significant amount of force to dislocate an elbow. This type of injury can occur while playing contact sports (football or soccer) or when falling on an outstretched arm from a significant height (pole vaulter, upended basketball player). Athletes can sustain this type of injury in a number of other sports including wrestling, gymnastics, rollerblading, skateboarding, and cheerleading.
Causes of dislocated elbow
The mechanism of injury for a dislocated elbow is most commonly a hyperextension injury or a sudden, violent medial force on the elbow that drives the ulna backward.
Treatment for dislocated elbow
The immediate treatment of an athlete suspected of having a dislocated elbow involves calling emergency medical services and stabilizing the athlete by immobilizing the elbow and treating for shock. Although there are several types of shock, the one that can be fatal is hemorrhaging from an open wound. If there is an open fracture involved, profuse bleeding may be possible.
The first priority for the caregiver is to stop the bleeding by applying direct pressure. If there is no bleeding, ice can be applied to help reduce swelling and inflammation. The athlete should be kept calm through quiet conversation focused on keep the athlete’s mind off of the injury.
If possible, the athlete should not be permitted to look at the injury especially if there is gross deformity. The athlete should not be moved from his/her original position, but be kept still until medical help arrives. Reducing a dislocated elbow should never be tried by anyone other than a physician.
If possible, an x-ray should be taken prior to reduction. A closed reduction may be performed under general or local anesthesia. If fractures are involved, internal fixation through surgery may be necessary to stabilize the fractured bones.
More Information: Read about sports injury treatment using the P.R.I.C.E. principle – Protection, Rest, Icing, Compression, Elevation.
In cases of simple dislocations, the elbow may be immobilized for one to two weeks to allow the injured ligaments to start to scar down. While the arm is immobilized, the athlete can perform isometric exercises such as ball squeezes (squeezing a tennis ball) to keep the muscles active and prevent atrophy of the muscles of the arm and forearm. Ball squeezes can be performed (10-15 repetitions) every waking hour.
Once the athlete is permitted to move the elbow, gentle strengthening exercises can be performed to strengthen the muscles of the upper arm (biceps, triceps) and forearm (muscles that move the wrist, hand, fingers, and thumb. The athlete should also focus on regaining full range of motion of the elbow including the motions of flexion, extension, pronation, and supination.
Under the supervision of a sports medicine professional, advanced exercises can be started once full range of motion has been achieved. These exercises focus on increasing the strength of all of the muscles most involved in the actions of the elbow, wrist, and hand. Power exercises can be initiated once full strength has been achieved.
Once cleared by his/her physician, sports-specific functional exercises can be started utilizing a careful progression working from simple to complex movements and from low intensity to high intensity. These programs can be designed by a sports medicine professional.
Possible long-term complications include:
• Limitation of full extension due to the formation of scar tissue
• Myositis ossificans or calcification of soft tissues around elbow (both restrict ability to straighten elbow)
• Ulnar nerve entrapment caused by scar tissue
However, even with rehabilitation, it is not uncommon for the athlete to not have full extension (ability to straighten the elbow all the way) for even two to three years post-injury. According to Bahr, R. & Maehlum, S. (2004), up to 50% of all dislocations may result in reduced range of motion, strength, pain, or instability.
When can I return to sports?
Once the athlete has pain-free range of motion, full strength, and has completed sport-specific functional training, the athlete may be released by his/her physician to return to sports. Even if there is a slight extensor lag, athletes can tolerate a slight limitation of extension in most sports.
Get a Virtual Sports Specialized appointment within 5 minutes for $29
 When you have questions like: I have an injury and how should I manage it? How severe is it and should I get medical care from an urgent care center or hospital? Who can I talk to right now? SportsMD Virtual Urgent Care is available by phone or video anytime, anywhere 24/7/365, and appointments are within 5 minutes. Learn more via SportsMD’s Virtual Urgent Care Service.
When you have questions like: I have an injury and how should I manage it? How severe is it and should I get medical care from an urgent care center or hospital? Who can I talk to right now? SportsMD Virtual Urgent Care is available by phone or video anytime, anywhere 24/7/365, and appointments are within 5 minutes. Learn more via SportsMD’s Virtual Urgent Care Service.
References
- Anderson, M.K., Hall, S. & Martin, M. (2005). Foundations of Athletic Training: Prevention, Treatment, and Management. (3rd Ed.). Lippincott Williams & Wilkins: Philadelphia, PA.
- Bahr, R. & Maehlum, S. (2004). Clinical Guide to Sports Injuries. Human Kinetics: Champaign, IL.
- Brukner, P. & Khan, K. (2002). Clinical Sports Medicine. (2nd Ed.). McGraw Hill: Australia.
- Irvin, R., Iversen, D. & Roy, S. (1998). Sports Medicine: Prevention, Assessment, Management, and Rehabilitation of Athletic Injuries. Allyn and Bacon: Needham Heights, MA.

