Patellar Tendonitis
Last Updated on August 12, 2024 by The SportsMD Editors
What is patellar tendonitis?
Patellar tendonitis is defined by inflammation in the patellar tendon, and most commonly occurs at its origin just below the kneecap. The most common cause is overuse or repetitive injury, and it has been reported to occur in athletes of virtually every sport. However, jumping activities place particularly high strains on the tendon and the condition is therefore more common in basketball players, tennis players, volleyball players, track and field athletes, as well as soccer players. With repetitive jumping, small, often “microscopic” tearing and injury of the tendon can occur. The chronic injury and healing response results in inflammation and localized pain. Many well-known elite athletes, including Brandon Inge of the Tigers, Oliver Perez of the Mets, and tennis star Rafa Nadal have fought chronic battles with patellar tendonitis during their career. Rarely, acute patellar tendonitis can develop in response to a single traumatic event and should raise concern regarding a partial or complete tendon rupture.
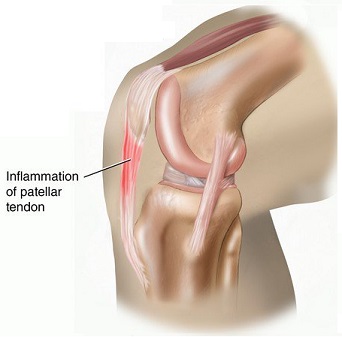 The patellar tendon is a thick, organized band of tissue that attaches the kneecap (“patella”) to the shinbone (tibia). It plays a crucial role in transmitting the forces generated by the muscles in the front on the thigh (“quadriceps”) to the tibia so that the leg can be straightened and support our weight with walking or jumping. The patellar tendon together with the quadriceps muscle, quadriceps tendon, patella, and its surrounding tissue (“retinacula”) make up the extensor mechanism of the knee. The patellar tendon is composed of a highly organized arrangement of collagen that is organized longitudinally to resist tensile forces like a rope.
The patellar tendon is a thick, organized band of tissue that attaches the kneecap (“patella”) to the shinbone (tibia). It plays a crucial role in transmitting the forces generated by the muscles in the front on the thigh (“quadriceps”) to the tibia so that the leg can be straightened and support our weight with walking or jumping. The patellar tendon together with the quadriceps muscle, quadriceps tendon, patella, and its surrounding tissue (“retinacula”) make up the extensor mechanism of the knee. The patellar tendon is composed of a highly organized arrangement of collagen that is organized longitudinally to resist tensile forces like a rope.
Patellar Tendonitis Symptoms
The diagnosis of patellar tendonitis is usually straightforward. Pain is usually reproduced with palpation of the area of inflammation and injury. This is most commonly at the inferior pole of the patella, but can occur anywhere along the course of the tendon. Compared to the opposite, normal knee, the tendon will often appear swollen and often warm to the touch. Depending on the severity, the athlete may have significant pain with jumping or kneeling. Walking up and down stairs can also place significant loads on the extensor mechanism and exacerbate the pain.
X-rays are sometimes useful to evaluate for other causes of knee pain but are typically normal with patellar tendonitis. If the patellar tendon is ruptured, the kneecap will displace “upward” and the distance between the kneecap and shinbone is greater than normal (“patella alta”). Ultrasonography and MRI are both sensitive and specific in identifying patellar tendinitis and localizing the area of “micro-injury” to the tendon.
Increase risk of patellar tendonitis
The cause of patellar tendonitis in athletes is often multifactorial. However, some factors that may increase the risk of this injury include:
• Overuse – particularly with recurrent jumping activities.
• Inadequate conditioning or stretching – an abnormal length-tension relationship and compliance of the thigh and calf muscles can increase strain on the patellar tendon and increase the risk of injury.
• Obesity – small increases in weight place dramatically increased stress on the kneecap and extensor mechanism. In fact, a gain of one pound can manifest as 8 to 10 more pounds of force on the knee with certain activities.
• Patella alta – a “higher than normal” kneecap position may increase the strain and risk of injury to the patellar tendon.
Prevention
Unfortunately, it is hard to anticipate the development of patellar tendonitis. However, as with most overuse injuries, routine stretching before strenuous competition can help to prevent injury. Stretching the quadriceps, hamstrings, and calf muscles helps to minimize the risk of eccentric, injurious loads on the tendon during running or jumping activities.
Patellar Tendonitis Treatment
The first line of treatment of patellar tendonitis in athletes is typically nonoperative. Initially, sports injury treatment using the P.R.I.C.E. principle – Protection, Rest, Icing, Compression, Elevation can be applied to patellar tendonitis.
It is critical that the athlete avoid the provocative activities that are causing pain. Typically, this means a cessation of competition and period of rest from running and jumping activities. This will decrease the strain and prevent recurrent injury to the tendon.
Icing and use of nonsteroidal anti-inflammatory medications (NSAIDs) can certainly help to alleviate the pain, and may be a useful augment to physical therapy and stretching exercises during the healing and recovery phase.
Tendonitis can be successfully treated but it is important to note that the treatment protocol for tendonitis is unique and different than treating other acute injuries. The wrong treatment can exacerbate the condition increasing the time for recovery. To learn more, click the following link on treating tendonitis.
Patellar Tendonitis Exercises
As the pain resolves after a period of rest, gentle stretching and strengthening exercises are initiated. These exercises for patellar tendonitis help to restore the normal length-tension relationship or the muscles and tendons, and also play a crucial role in preventing a recurrence of patellar tendinitis. It is of tantamount importance to learn proper jumping and landing techniques, and to strengthen the muscles around the kneecap to reduce the forces on the tendon itself. Eccentric strengthening exercises of the quadriceps muscles have been shown to be particularly effective – these are exercises that involve muscle contraction while lengthening; for example, lowering a weight in a controlled fashion from an extended to flexed knee position.
Self Message Techniques
Steroid injections
Steroid injections are generally NOT recommended for the treatment of patellar tendonitis. While they can certainly decrease local inflammation at the site of injury, the injections must be approached caution as the steroid medication can weaken the tendon and increase the risk of patellar tendon rupture.
Taping or bracing patellar tendonitis
Taping or use of a patellar tendon “strap” brace has often provided significant relief to athletes, although the success is quite variable. The precise mechanism of action is unknown, but it is believed that taping or bracing alters the angle and direction of stress at the site of injury, effectively “unloading” this region and decreasing the pain by distributing forces away from the tendon. A Chopat strap has been specifically used to unload the patellar tendon for both patellar tendonitis and Osgood-Schlatter’s Disease.
Other treatment options short of surgery
A number of other treatments have been used with variable success in the treatment of patellar tendinitis. These include:
Platelet-Rich Plasma (PRP): PRP injection has recently been used in the treatment of chronic, refractory tendonitis. PRP is derived from the patient’s own blood and concentrates many important growth factors that have been shown to be important in the body’s healing response following injury. Preliminary results have been encouraging, but long-term success remains unknown.
Extracorporeal Shock Wave Therapy (ECW): ECW uses sound waves to stimulate healing at the injured tendon. It has been used with modest success in the treatment of tendinitis and plantar fasciitis.
Laser & Electrical Stimulation: While the mechanism of action is unclear, laser and electrical stimulation techniques have been reported with good success in small case series.
Patellar Tendonitis Surgery
Patellar tendonitis surgery is indicated in severe cases of patellar tendonitis that fail to resolve with conservative measures. The operation is directed at repairing viable tendon tissue and debriding away severely damaged tendon, usually just below the kneecap. Many elite athletes, including Brandon Inge, Oliver Perez, and Carlos Beltran, have undergone this surgery and successfully returned to MLB competition.
Get a Virtual Sports Specialized appointment within 5 minutes for $29
 When you have questions like: I have an injury and how should I manage it? How severe is it and should I get medical care from an urgent care center or hospital? Who can I talk to right now? SportsMD Virtual Urgent Care is available by phone or video anytime, anywhere 24/7/365, and appointments are within 5 minutes. Learn more via SportsMD’s Virtual Urgent Care Service.
When you have questions like: I have an injury and how should I manage it? How severe is it and should I get medical care from an urgent care center or hospital? Who can I talk to right now? SportsMD Virtual Urgent Care is available by phone or video anytime, anywhere 24/7/365, and appointments are within 5 minutes. Learn more via SportsMD’s Virtual Urgent Care Service.
Quadriceps vs Patellar Tendonitis, Strengthening in New Mobility, Analgesic Creams https://t.co/anhqeZCU8F pic.twitter.com/TcOErYQN7H
— Mike Reinold (@mikereinold) May 20, 2019
Official: Plizzari underwent surgery to deal with chronic bilateral patellar tendonitis, out for three months https://t.co/y7UqkGGvQ9
— Meytar Zeevi (@RossoneriBlog) September 22, 2021

