Medial Collateral Ligament Injury (MCL)
Last Updated on August 12, 2024 by The SportsMD Editors
Medial collateral ligament injuries to the knee are not uncommon. Many well-recognized professional athletes, including Jay Cutler, Hines Ward, Knowshan Moreno, and Troy Polamalu, have suffered from a medial collateral ligament tears after injury on the football field. These can occur alone or in combination with other ligament or cartilage injuries of the knee in athletes.
What is the medial collateral ligament (MCL)?
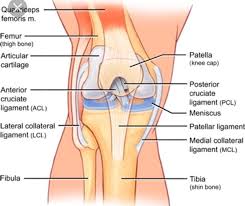 The Medial Collateral Ligament (MCL), is critical to the stability of the knee joint. The MCL is a fibrous band of tissue made up of collagen fibers that run along the inner aspect of the knee from the end of the thigh bone (femur) to the top of the shin bone (tibia). In this location, the MCL provides “side-to-side” stability to the knee and prevents widening of the inner aspect of the joint with forces applied to the outside aspect of the knee (valgus force). When significant forces are applied to the outside aspect of the knee, as can occur during a tackle in football or awkward slide into base with baseball, the ligament can be stretched (“sprained”) or torn.
The Medial Collateral Ligament (MCL), is critical to the stability of the knee joint. The MCL is a fibrous band of tissue made up of collagen fibers that run along the inner aspect of the knee from the end of the thigh bone (femur) to the top of the shin bone (tibia). In this location, the MCL provides “side-to-side” stability to the knee and prevents widening of the inner aspect of the joint with forces applied to the outside aspect of the knee (valgus force). When significant forces are applied to the outside aspect of the knee, as can occur during a tackle in football or awkward slide into base with baseball, the ligament can be stretched (“sprained”) or torn.
The MCL is made up of a superficial and a deep layer. The superficial MCL runs from the distal femur to the tibia 4 or 5 centimeters below the knee joint line, and is found just below the sheath of the sartorius muscle tendon. The deeper MCL layer lies just outside of the knee capsule and inserts directly into the tibial plateau and medial meniscus. The superficial layers are much more mechanically important in resisting forces to the outside aspect of the knee (“valgus” force).
Causes
Because the MCL resists widening of the inside of the knee joint, the MCL is usually injured indirectly by traumatic forces in the outside of the knee. These are certainly common in contact sports from tackles or “clipping injuries” in football and soccer. However, MCL injuries can also occur from noncontact mechanisms such as awkward landing or pivoting events in basketball or slides into base with baseball. An MCL tear or sprain can occur in isolation or in combination with injury to the meniscus, cartilage, or cruciate ligaments.
Symptoms and Classifications of Medial collateral ligament (MCL)
The most common symptom following an MCL injury is pain directly over the medial aspect of the knee. The MCL can be tender to palpation over its attachment to the thighbone (femur) proximally, at its mid-substance, or distally over the shin bone (tibia) depending on the location of injury. The pain may also be reproduced by stressing the knee with a force applied to the outside aspect of the knee (“valgus force”), attempting to widen the inner aspect of the joint and stress the MCL. While a valgus force is applied, the inner aspect of the joint line can be palpated – widening that is 5 to 10mm greater than the normal, uninjured knee is significant for MCL injury. Swelling over the torn ligament may appear, and bruising or general swelling of the joint is not uncommon. In more severe injuries, patients may complain that the knee is unstable and feel as though their knee may ‘give out’ or buckle.
Based on physical examination, MCL injuries are graded in severity on a scale of I to III.
Grade I Medial collateral ligament tear (MCL)
Injuries are incomplete tears of the MCL. The ligament is still intact but stretched, and the symptoms are mild. Patients usually complain of pain with palpation of the MCL.
Grade II Medial collateral ligament (MCL)
MCL tear is a partial or incomplete tear. There is significant pain with valgus stress of the knee and palpation along the medial aspect of the knee over the ligament. Athletes with these tears often complain of knee pain or instability when attempting to cut or pivot.
Grade III Medial collateral ligament (MCL)
Tears are complete tears of the MCL. These athletes have significant pain along the medial aspect of the knee. Even deep bending of the knee is uncomfortable. These tears often occur in combination with other injuries in the knee, and complaints of “giving out” or instability with walking, running, or pivoting are common. A knee brace or a knee immobilizer is usually needed for comfort.
Imaging studies with an MCL tear
Plain radiographs can sometimes be helpful with MCL injuries. When the ligament has torn off the thigh bone (“femoral side”), it often tears with a piece of bone that is visible on x-ray. With old or recurrent injuries to the femoral side of the MCL, calcification at its origin can develop – this has been termed the “Pellegrieni-Stieda” lesion. Under most circumstances, however, plain radiographs are most helpful in ruling out associated fractures with MCL injury.
MRI is the imaging study of choice to diagnose MCL tears. Injuries are readily identified on a “T2 sequence” that shows loss of continuity of the ligament and surrounding blood and fluid from the injury. The MRI will also localize the injury to the ligament to be proximal at the femur, in its mid-substance, or distally at the tibia.
Treatment for Medial collateral ligament
Medial collateral ligament treatment for an athlete rarely requires surgical intervention. Usually rest and anti-inflammatory medications followed by rehabilitation will allow patients to resume their previous level of activity. All MCL injuries, however, are not created equal. Therefore, the time for an athlete to return-to-play is highly variable and dependent on the severity of the injury.
Grade I injuries usually resolve without complication. They are typically managed with rest, ice, and nonsteroidal anti-inflammatory medications until the knee is pain-free to examination or routine activities. Most athletes with a grade I MCL tear will be able to return to their sport within 1-2 weeks following their injury.
When a grade II MCL tear occurs, a hinged knee brace is commonly used to protect the knee from valgus forces. Nonoperative treatment also ensues with icing, nonsteroidal medications, and controlled rehabilitation. Athletes with a grade II injury can return to activity once they are not having pain to palpation or stressing of the MCL with a valgus force. Athletes can often return to sports within 3-4 weeks after their injury, but may remain in a protective hinged brace with contact sports.
When a grade III injury occurs, the pain usually significant in the acute post-injury period. Athletes usually require a hinged brace locked in extension and crutches to protect against weightbearing for 1 to 2 weeks. As the pain resolves, the brace can be unlocked to allow range-of-motion as tolerated. Gradual weightbearing can be initiated as well. Once the athlete can comfortably flex the knee to 100 degrees, elliptical and stationary bicycle riding can begin. Light running can begin once the athlete has regained their quadriceps strength compared to the opposite side, and sporting activity can follow as long as the athlete remains pain-free. Complete rehabilitation from a grade III MCL tear can range from 6 weeks to 4 months.
More Information: Read about sports injury treatment using the P.R.I.C.E. principle – Protection, Rest, Icing, Compression, Elevation.
Surgery for Medial collateral ligament
Most medial collateral ligament tears of the knee do not require surgery and will heal with time and rehabilitation. However, some severe Grade III MCL tears will not heal and residual instability with “opening of the joint” to stress on the outside aspect of the joint (“valgus force”) can persist. These type of MCL injuries are frequently seen in combination with associated ACL tears or high-energy, knee dislocation injuries. Rarely, the ligament stump can retract and become trapped within the joint. When this is seen on MRI, surgical intervention and repair are usually required to restore the normal anatomy. Consultation with a sports medicine doctor is important to examine and monitor the progress of a healing MCL injury. If surgery is required, a ligament repair with or without reconstruction with a tendon graft may be performed depending on the location and severity of the injury.
What about platelet-rich plasma (PRP) injections for MCL injury in an athlete?
PRP injections have been increasingly utilized in the treatment of various soft tissue injuries in athletes. It is thought that the isolated “healing factors” from the athlete’s own blood may accelerate or stimulate healing at the site of injury. This treatment was used in the treatment of Hines Ward’s MCL injury during football season. While this treatment may prove to be effective, studies are currently in progress to evaluate its efficacy.
Get a Virtual Sports Specialized appointment within 5 minutes for $29
 When you have questions like: I have an injury and how should I manage it? How severe is it and should I get medical care from an urgent care center or hospital? Who can I talk to right now? SportsMD Virtual Urgent Care is available by phone or video anytime, anywhere 24/7/365, and appointments are within 5 minutes. Learn more via SportsMD’s Virtual Urgent Care Service.
When you have questions like: I have an injury and how should I manage it? How severe is it and should I get medical care from an urgent care center or hospital? Who can I talk to right now? SportsMD Virtual Urgent Care is available by phone or video anytime, anywhere 24/7/365, and appointments are within 5 minutes. Learn more via SportsMD’s Virtual Urgent Care Service.
References:
Indelicato, PA. “Isolated Medial Collateral Ligament Injuries in the Knee” J. Am. Acad. Ortho. Surg., Jan 1995; 3: 9 – 14.
Grood E et al. Ligamentous and capsular restraints preventing straight medial and lateral laxity in intact human cadaver knees. J Bone Joint Surg 1981; 63A:1257-1269.

